Today, there are various weight loss surgeries available, researching which one is right for you can be overwhelming, as each procedure is tailored to suit specific patients needs and goals. The cutting edge procedures offered at Renew Bariatrics by our expert surgeons are performed to aid patients with sustainable weight loss results.
Both Biliopancreatic Diversion with duodenal switch and Roux-en-Y gastric bypass surgeries are advanced weight loss surgeries we perform that have been shown by different studies to be effective in morbidly obese individuals in achieving weight loss and resolution of the disease conditions that are associated with obesity. So, let’s discuss gastric bypass vs. duodenal switch surgeries.
Roux-en-Y gastric bypass surgery used to be the most commonly performed weight loss surgery in the United States but has now been overcome by gastric sleeve surgery. Duodenal switch, on the other hand, is mostly reserved for super obese individuals (BMI≥ 50kg/m2) or as a revision surgery following the failure of other weight loss surgeries.
Following recovery from anesthesia, the other major issue is a pain. Pain usually originates from the sites of incisions (port sites). The most significant port causes the highest pain because it is the incision made to allow removal of the resected part of the stomach. During the procedure, this most considerable incision is stretched to provide adequate space for the resected part of the stomach. This pain can be efficiently managed by sufficient analgesia to ensure a pain-free post-operative period. Initially, the analgesics will be parenteral before converting them to oral once you start taking orally.
Renew Bariatrics recommends Gastric Bypass Surgery for a majority of reasons, primarily that it provides very high expected weight and reduction in comorbidities. Duodenal Switch (DS) is not as well-researched as Gastric Bypass Surgery (RNY); which can promote unexpected outcomes. DS also promotes extreme weight-loss, which can cause serious health issues.
Interested in Gastric Bypass Surgery in Mexico? Learn more about undergoing Gastric Bypass in Tijuana or Cancun, Mexico now. Call us today!
 |  |
|
|---|---|---|
| Gastric Bypass Surgery | Duodenal Switch | |
| Method of Weight Loss | Restrictive & Malabsorptive | Restrictive & Malabsorptive |
| Duration of Procedure | 2 Hour | 4 Hour |
| Length of Hospital Stay | 2-3 Nights | 2-3 Nights |
| Estimated Weight Loss | 70% of Excess Weight | 65-90% of Excess Weight |
| Weight Loss at 1 Year | 60-80% | 70% |
| Comorbidities | Higher Resolved | Significant Resolved Rates |
| Hypertension Resolved | 69% | 43% |
| Diabetes Resolved | 83% | 92-100% |
| Migrations Resolved | 57% | Major Improvements |
| GERD Resolved | 80% | 49% |
| Mortality | 0.3% | |
| Asthma | 80% | 90% |
| Sleep Apnea | 98% | 85% |
| Depression | Most Resolved | 57% |
| Quality of Life Improved | 95% | 95% |
| Common Complications | Anastomotic Leaks 5% | N/A |
| Common Side Effects | Nausea, Digestive Issues | GERD, Gallstone, Bowel Movement |
| Recovery | 2 to 4 Weeks | 2 to 4 Weeks |
| Cost: Self-Pay Average | $25,000 | $30,000 |
| Cost w/ Renew Bariatrics | $6,299 | Not Offered |
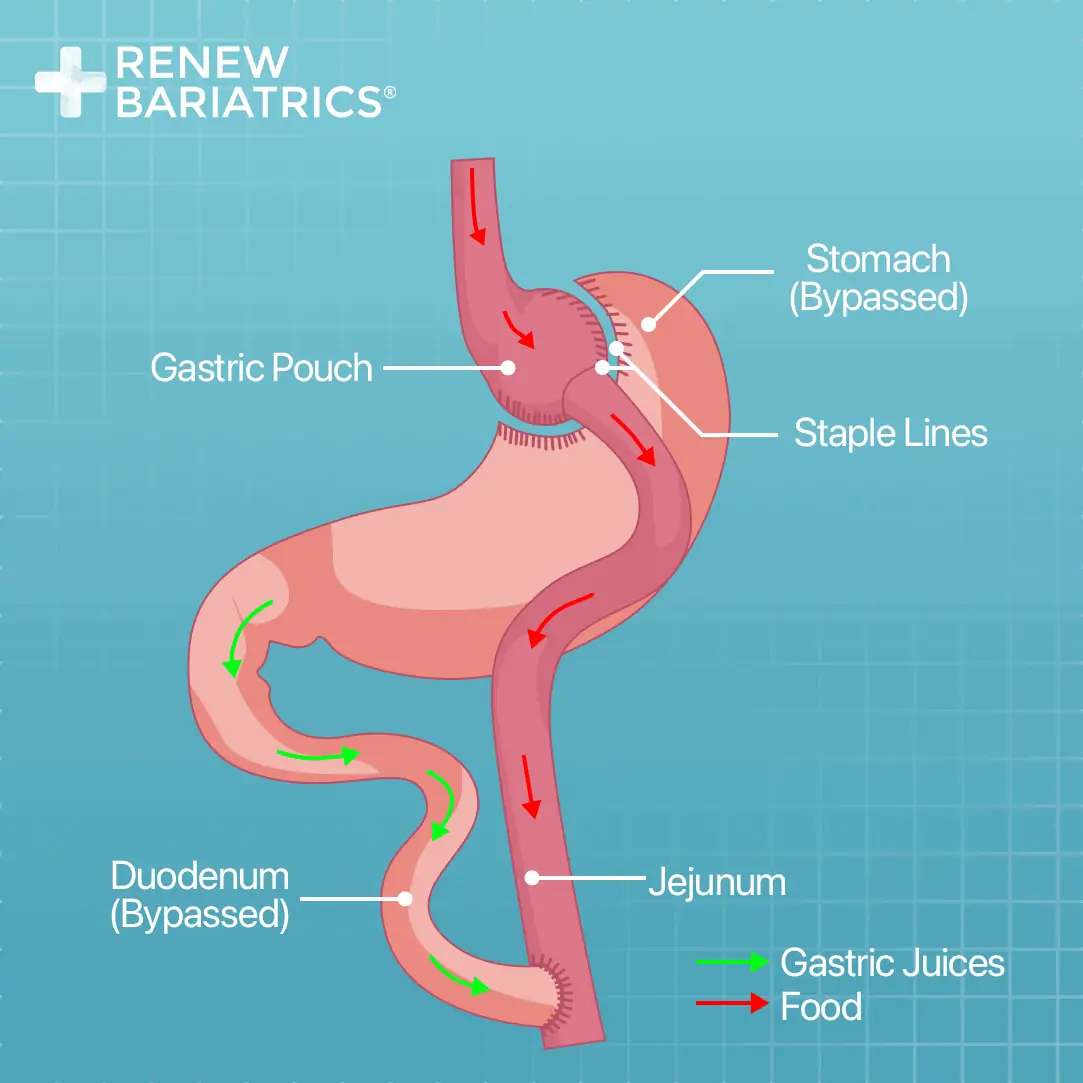
Both duodenal switch and gastric bypass combine restrictive and malabsorptive mechanisms to induce weight loss. In the case of Roux-en-Y gastric bypass, a small pouch is created from the upper part of the stomach; this serves as the new stomach. The small intestine is then divided at about 45cm from the stomach, and the lower end is joined to the new stomach while the upper end is joined to the intestine at about 100cm from the point of division.
With the above arrangement, the remaining larger portion of the stomach is bypassed, and absorption will not take place in most of the initial part of the small intestine (due to incomplete digestion). This is because pancreatic enzymes and bile will only come in contact with the food after the first 100cm of the small
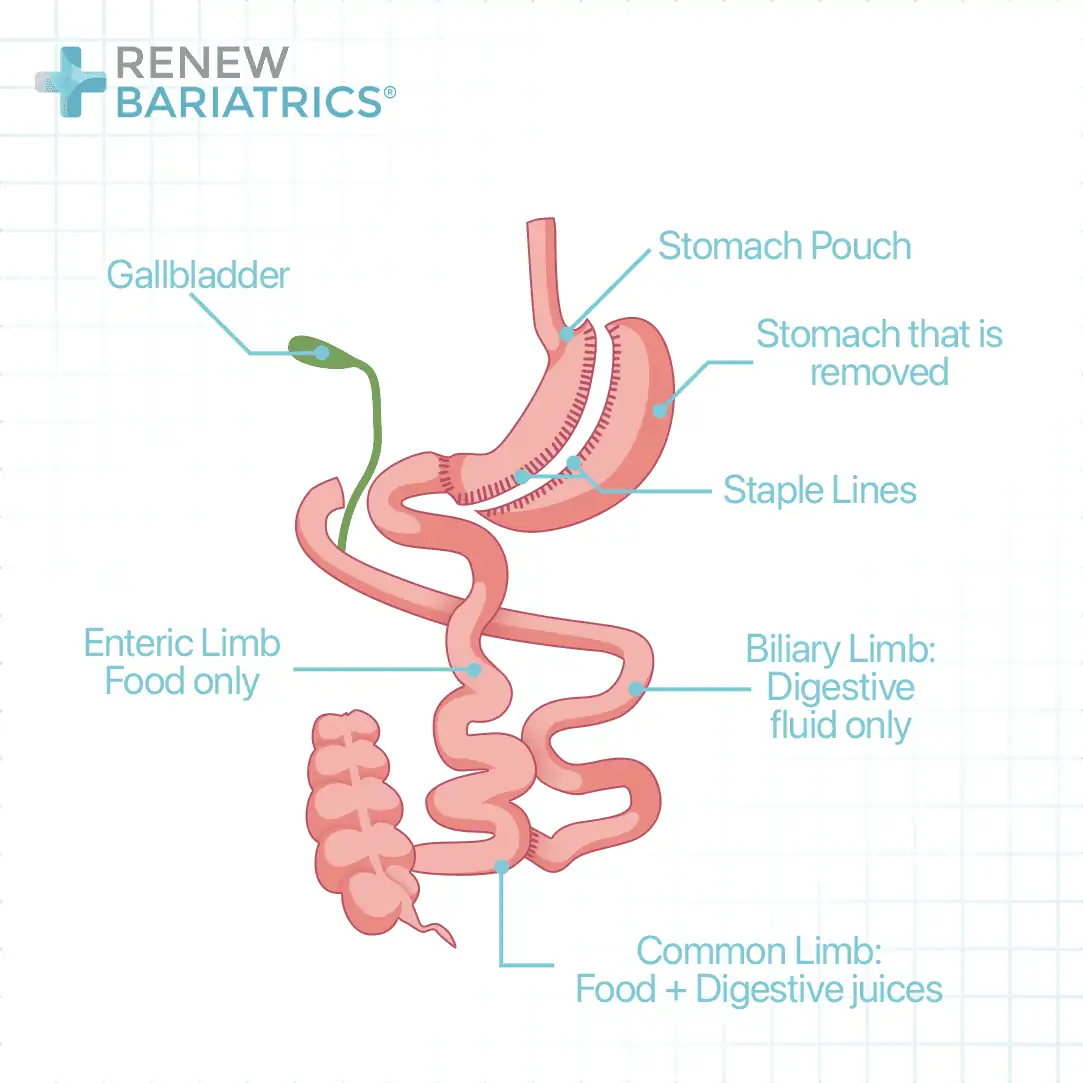
In a duodenal switch, the capacity of the stomach is also reduced by a gastric sleeve surgery. The intestine is then refashioned in such a way as to prevent the bile and pancreatic enzymes from coming in contact with the food until about 50cm from the junction between the small and the large intestine.
This is achieved by dividing the duodenum (1st part of the small intestine). The lower end of the gap is closed and turned to a blind end. The small intestine is again divided at the about 250cm from where it joined the large intestine. The upper end is joined to the small intestine at about 50cm from where it entered the large intestine. The lower end is joined to the upper end of the first point of division. With this arrangement, absorption will not take place in a relatively longer part of the intestine than what obtains in gastric bypass.

Both gastric bypass and duodenal switch can be done by open surgery or laparoscopic approach. The laparoscopic approach is favored as it reduces the perioperative complications. The operative duration of the duodenal switch is longer than that of gastric bypass surgery with a difference of up to an hour. Patients also stay more in the hospital after duodenal switch than after gastric bypass with a difference of about one day.
Duodenal switch is costlier than gastric bypass. Although cost varies by countries and hospitals, the average cost of the duodenal switch in the U.S. is $25,000 ($23,000-$34,000) while that of gastric bypass surgery is $21,000 ($17,000-$30,000). While most insurance policies cover gastric bypass surgery, only a few companies provide coverage for duodenal switch.
The percentage of excess weight loss after gastric bypass surgery is lesser than that of duodenal switch. Rabkin reported percentage excess weight loss of 78% vs. 74% in favor of the duodenal switch. [3] On an average, the patient can lose about 78% of the excess weight by 18months of the duodenal switch and about 70% of the excess weight after gastric bypass surgery. Patients also experience a higher percentage of total body weight loss after duodenal switch than after gastric bypass surgery.
In the work of Mingrone et al., a remission of type 2 diabetes mellitus was reported in 95% and 75% of patients after the duodenal switch and gastric bypass respectively at 2years post-surgery. [4] A higher percentage of resolution of other comorbid conditions in favor of duodenal switch has also been reported by various studies.
Duodenal switch is associated with more complications and a higher risk of death than gastric bypass surgery. [5] However, almost all complications that can be seen with the duodenal switch can also occur after gastric bypass surgery (except for heartburn from GERD). Nutritional deficiency is more severe with duodenal switch. Also, complications such as deep vein thrombosis (clotting of blood in the leg veins) and pulmonary embolism (obstruction of the blood vessels in the lungs by a blood clot) are commoner with duodenal switch.
In summary, the comparison between the duodenal switch and gastric bypass surgery is shown in the table below:
Parameters | Duodenal switch (BPD-DS) | Gastric bypass surgery |
Mechanism of weight loss | Restrictive and malabsorptive | Restrictive and malabsorptive |
Duration of procedure | Shorter | |
Length of hospital stay | Shorter | |
Cost | Lower | |
Estimated weight loss | Higher | |
Reversal of comorbid conditions | Higher | |
Risk of complications | Lower (except heartburn) | |
Risk of death | Lower |
In conclusion, duodenal switch and gastric bypass are weight loss surgeries that combine both restrictive and malabsorptive mechanisms to induce weight loss. Both have almost the same types of complications. However, the risk is higher after duodenal switch. While gastric bypass is cheaper and safer, duodenal switch achieves more weight loss and reversal of comorbid conditions.
Contact our helpful patient educators who can help guide you through the entire process of getting approved for the Bariatric Surgery Mexico.